Image
Best Practice magazine
A journal of dentistry, business and policy that shines a spotlight on Delta Dental network dentists.
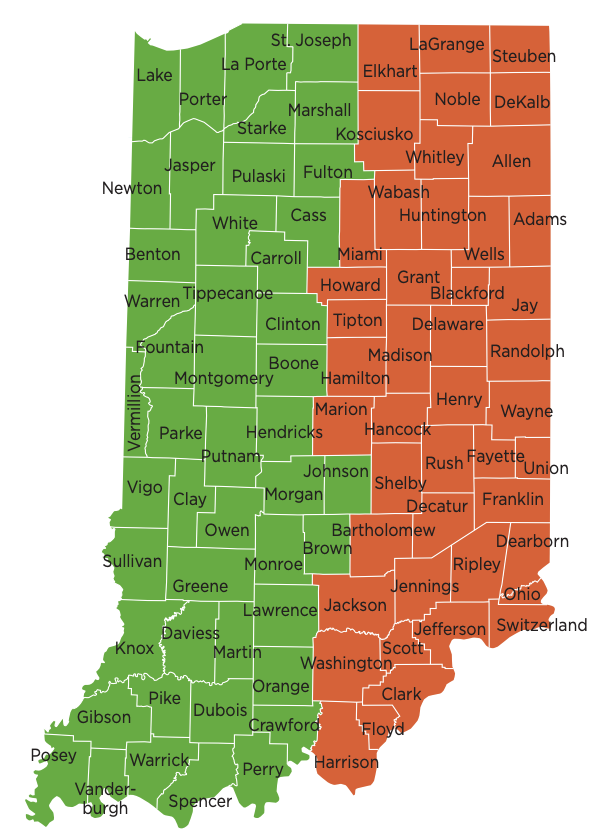
Do you know your provider representative?
Check out the map and reach out today!
Image

Image

Counties by representative
- Benton
- Boone
- Brown
- Carroll
- Cass
- Clay
- Clinton
- Crawford
- Daviess
- Dubios
- Fountain
- Fulton
- Gibson
- Greene
- Hendricks
- Jasper
- Johnson
- Knox
- La Porte
- Lake
- Lawrence
- Marshall
- Martin
- Monroe
- Montgomery
- Morgan
- Newton
- Orange
- Owen
- Parke
- Perry
- Pike
- Porter
- Posey
- Pulaski
- Putnam
- St. Joseph
- Starke
- Spencer
- Sullivan
- Tippecanoe
- Vanderburgh
- Vermillion
- Vigo
- Warren
- Warrick
- White
- Adams
- Allen
- Bartholomew
- Blackford
- Clark
- Dearborn
- Decatur
- Delaware
- DeKalb
- Elkhart
- Fayette
- Floyd
- Franklin
- Grant
- Hamilton
- Hancock
- Harrison
- Henry
- Howard
- Huntington
- Jackson
- Jay
- Jefferson
- Jennings
- Kosciusko
- LaGrange
- Madison
- Marion
- Miami
- Noble
- Ohio
- Ripley
- Rush
- Scott
- Shelby
- Steuben
- Switzerland
- Tipton
- Union
- Wabash
- Washington
- Wayne
- Wells
- Whitley